Plantar Fasciitis Treatment: Symptoms, Causes & Proven Relief
Medically reviewed by Dr. Neelabh, MS (Orthopedics)Educational information only—always consult a qualified Orthopedic specialist for diagnosis and treatment.
Plantar fasciitis is the most common cause of heel pain. It typically presents as sharp pain with the first steps in the morning or after sitting, which often eases with movement and may return after prolonged activity. The condition is frequently degenerative (fasciosis) rather than purely inflammatory, and the vast majority of people improve without surgery. This plantar fasciitis treatment guide explains proven steps to relieve heel pain.
On this page
- Watch: Dr. Neelabh Explains Plantar Fasciitis Treatment
- What is Plantar Fasciitis?
- Common Causes and Risk Factors
- Symptoms You Shouldn’t Ignore
- Diagnosis (and Look-Alikes to Rule Out)
- Plantar Fasciitis Treatment Pathway (Step-by-Step)
- What to Expect at Your Consultation
- Plantar Fasciitis Treatment FAQs
Watch: Dr. Neelabh Explains Plantar Fasciitis Treatment
What is Plantar Fasciitis?
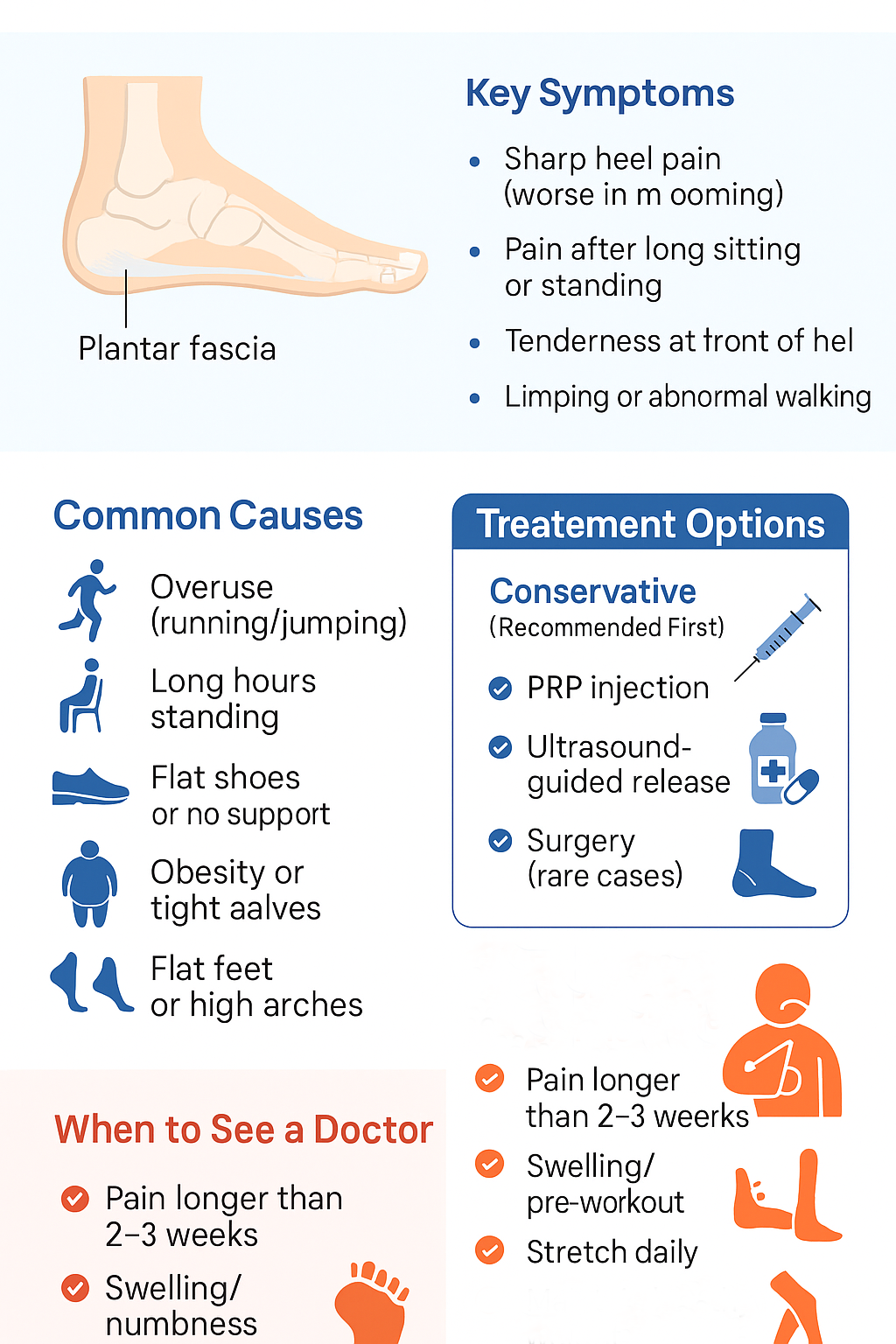
The plantar fascia is a thick, fibrous band of tissue that runs along the bottom of your foot, connecting your heel bone to your toes. It supports the arch and absorbs shock. Repeated micro-strain can cause degenerative changes (fasciosis) and pain at the fascia’s attachment to the heel bone, usually on the inner side (medial calcaneal tubercle).
Common Causes and Risk Factors
- Training/Load Errors: A sudden increase in running, jumping, or prolonged standing.
- Surfaces & Footwear: Long hours on hard surfaces, walking barefoot on tiles, or wearing unsupportive, worn-out shoes.
- Biomechanical Factors: Tight calf muscles, limited ankle dorsiflexion, flat feet (pronation), or very high arches.
- Other Factors: Being overweight, occupational demands (e.g., teachers, factory workers).
Symptoms You Shouldn’t Ignore
- First-Step Pain: Sharp, stabbing pain in the heel with the first steps in the morning or after a period of rest.
- Point Tenderness: Pain localized to the bottom and inner side of the heel.
- Post-Activity Pain: The pain often improves during activity but returns afterward.
- Limping: An altered walking pattern to avoid putting pressure on the heel.
Diagnosis (and Look-Alikes to Rule Out)
- Clinical Exam: This is the cornerstone of diagnosis. We look for point tenderness at the medial heel and may perform a “Windlass test” (pain with passive big toe extension) to confirm. We also check for tight calf muscles.
- Imaging: Usually not required for a clear-cut diagnosis. An X-ray can rule out a stress fracture or a large heel spur, while an ultrasound can show fascia thickening. An MRI is rarely needed.
- Differential Diagnosis: It’s important to rule out other causes of heel pain, such as a calcaneal stress fracture, Baxter’s nerve entrapment, tarsal tunnel syndrome, or fat pad atrophy.
Plantar Fasciitis Treatment Pathway (Step-by-Step)
Our plantar fasciitis treatment plan is staged—reduce load, restore mobility, then rebuild strength and gradually return to impact.
1) First-Line Care (First 6–12 Weeks)
Consistency is key. The goal is to reduce load and improve tissue capacity.
- Load Management: Reduce high-impact activities (running, jumping) and avoid walking barefoot on hard floors.
- Plantar Fascia-Specific Stretch: While seated, cross the affected leg over the other knee and gently pull your big toe back toward your shin. Hold for 30 seconds, repeat 3–5 times, several times a day.
- Calf Stretching: Perform both straight-knee (gastrocnemius) and bent-knee (soleus) calf stretches daily.
- Supportive Footwear & Orthoses: Wear shoes with good arch support and a firm heel counter. Over-the-counter arch supports or silicone heel cups can be very effective.
- Taping: Low-Dye or arch taping can provide significant short-term pain relief.
- Night Splint: If first-step morning pain is severe and persistent, a night splint can help by keeping the fascia stretched overnight.
2) Progressive Strengthening (Starting around Week 4)
- High-Load Strength Training: Performing slow, controlled heel raises on a step with a towel rolled under the toes can help remodel the fascia.
- Foot Intrinsics: Exercises like towel curls and marble pickups strengthen the small muscles of the foot.
- Hip & Core Strengthening: Improving gluteal and core strength helps control lower limb mechanics.
A Surgeon’s Perspective by Dr. Neelabh
“Most heel pain gets better with the basics: stretching, footwear changes, and load management. Patience is key. Advanced treatments like shockwave or a carefully placed injection have a role, but surgery is very rarely needed and only considered after a long, structured non-operative program has failed. Consistency with your rehab plan is the best path to recovery.”
What to Expect at Your Consultation
- Detailed Discussion: A thorough review of your symptoms, activity levels, footwear, and treatment goals.
- Physical Examination: A comprehensive assessment to confirm the diagnosis and rule out other conditions.
- Imaging (If Needed): We will order an X-ray or ultrasound only if the diagnosis is unclear or there are red flags.
- Personalized Plan: You will leave with a clear, step-by-step plantar fasciitis treatment plan—starting with physio and orthoses and escalating to advanced options only if needed.
Plantar Fasciitis Treatment FAQs
What’s the difference between a heel spur and plantar fasciitis?
A heel spur is a bony growth on the heel bone. While often seen on X-rays of people with plantar fasciitis, the spur itself is rarely the source of pain. The pain comes from the fascia. We treat the fasciitis, not the spur.
What is the fastest way to treat plantar fasciitis?
The fastest plantar fasciitis treatment combines consistent plantar fascia and calf stretching, load management, and supportive footwear/orthoses. Most patients see significant improvement within 6–12 weeks.
Do I need injections or surgery?
Usually not. Over 90% of cases resolve with non-surgical care. Advanced options like shockwave therapy (ESWT) or a single, carefully guided corticosteroid injection may be considered for persistent cases. Surgery is a last resort.
Need Help with Heel Pain?
We follow an evidence-based, conservative-first plantar fasciitis treatment plan, with advanced options for persistent cases. Explore our Orthopedic services or book a consultation. Call/WhatsApp: +91‑9810117204.
Trusted Resources: AAOS: Plantar Fasciitis · JOSPT Clinical Practice Guideline · NHS: Heel Pain